- Call Us: 8828131345
- Email Us: kingshukganguly24@gmail.com
Dr. Kingshuk Ganguly
About Us
10+
Years of Experience
2.5K+
Arthroplasty Procedures Performed
5K+
Joint Replacements Done
25K+
Happy Patients
Our Specialization
Our Healthcare Services
Comprehensive diagnosis, surgical expertise, and personalized recovery plans
Dr. Kingshuk Ganguly
About Doctor
.png)
- MBBS (KEM Hospital, Mumbai) , MS Orthopedics (Gold Medallist), FIJR (Mumbai), Dip. FM (FIFA), Arthroscopic Training, Ganga Hospital ( Coimbatore)
- 10.0 Years Of Experience
- Licence No. 2020043015-MMC
- Call
- Video Call
- In person
Testimonials
What our Patients says about us
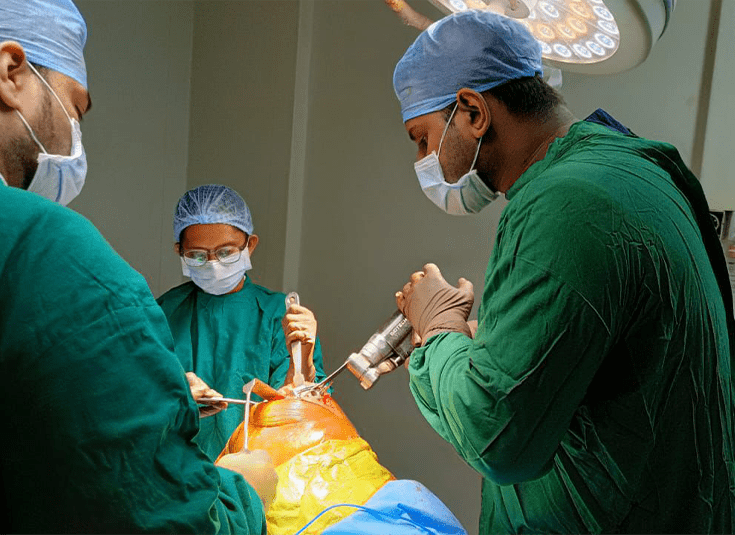
Media Pictures
Frequently Asked Questions
Dr. Kingshuk Ganguly is a highly skilled orthopedic surgeon based in Mumbai, India. He completed his MBBS at Seth GS Medical College and KEM Hospital, where he graduated with high honors. Dr. Ganguly pursued his MS in Orthopedics at K.S. Hegde Medical Academy in Mangalore, graduating as a gold medalist. Additionally, he has completed fellowships in joint replacement and sports medicine, gaining significant experience in robotic joint replacements and arthroscopic procedures.
Dr. Kingshuk Ganguly is an expert in communicating medical terminology clearly and concisely. He ensures that patients and healthcare professionals fully understand their treatment plans by explaining complex concepts in simple terms. His extensive experience in managing medical emergencies has honed his ability to foster positive relationships with patients and their families, making him a trusted and respected orthopedic surgeon in Mumbai.
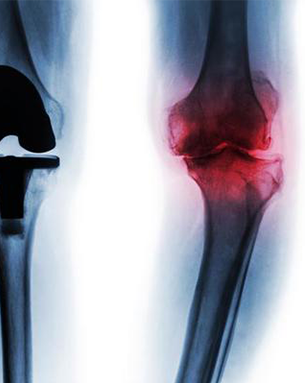
Arthroplasty is a surgical procedure where a damaged joint is replaced or reconstructed to restore function and relieve pain. It is often recommended for patients suffering from severe arthritis, such as knee osteoarthritis, or those with joint damage due to trauma or disease. Joint replacement surgery can significantly improve the quality of life for individuals with disabling joint pain and reduced mobility.
A joint replacement surgeon may recommend treatments for knee osteoarthritis ranging from conservative methods like physical therapy and medications to surgical interventions like knee arthroplasty. When conservative treatments fail to alleviate pain and improve function, knee arthroplasty, a type of joint replacement surgery, may be considered. This procedure involves replacing the damaged knee joint with an artificial implant to restore mobility and reduce pain.
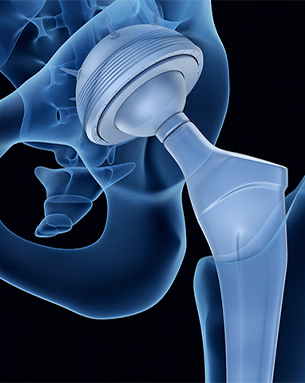
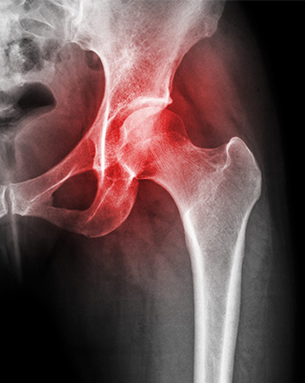
Hip avascular necrosis is a condition where the blood supply to the femoral head of the hip joint is disrupted, leading to bone tissue death and joint pain. Treatment can include non-surgical options like medications and physical therapy, but often requires joint replacement surgery or arthroplasty in advanced cases. A joint replacement surgeon may replace the damaged hip joint with a prosthetic to alleviate pain and restore function.
A: A minimally invasive spine specialist can play a crucial role in managing low back pain due to disc prolapse by offering a comprehensive approach to treatment. This can include physical therapy, exercises to strengthen the back muscles, and minimally invasive spinal procedures to relieve pressure on the affected disc. The goal is to alleviate pain, restore mobility, and prevent further injury, allowing patients to return to their active lifestyles.
Joint replacement surgery is generally considered necessary when conservative treatments like physical therapy, medications, and lifestyle modifications fail to relieve significant joint pain or when joint damage severely affects mobility and quality of life. Conditions such as severe knee osteoarthritis or hip avascular necrosis may necessitate this surgical intervention, where the damaged joint is replaced with an artificial prosthetic to restore function and alleviate pain.
A joint replacement surgeon manages trauma and fracture cases by assessing the extent of the injury and devising an appropriate treatment plan. This can include surgical interventions to realign and fixate fractures, as well as restorative procedures like joint replacement surgery in cases of joint damage. The goal is to ensure proper healing, restore function, and prevent long-term complications, allowing patients to regain mobility and return to their daily activities.
Minimally invasive spinal procedures are advanced surgical techniques aimed at treating spinal conditions with less tissue disruption than traditional open surgery. They involve smaller incisions and the use of specialized instruments, resulting in reduced postoperative pain, faster recovery, and lower risk of complications. These procedures are particularly beneficial for patients with conditions like disc prolapse, where quick recovery and minimal damage to surrounding tissues are crucial for maintaining mobility and quality of life.
Arthroplasty, or joint replacement surgery, typically involves a longer recovery period compared to less invasive treatments, as it requires significant healing and rehabilitation to ensure the artificial joint functions properly. However, advancements in surgical techniques and postoperative care have significantly reduced recovery times. Many patients experience substantial improvement in pain and mobility within weeks, and with proper rehabilitation, can return to many normal activities within months.
Post joint replacement surgery, it is essential to incorporate lifestyle changes that promote recovery and prolong the lifespan of the artificial joint. These may include engaging in regular low-impact exercises to improve strength and flexibility, maintaining a healthy weight to reduce joint stress, and avoiding high-impact activities that may damage the new joint. Following these guidelines can enhance the long-term success of joint replacement and improve overall quality of life.
Before considering arthroplasty for knee osteoarthritis, non-surgical treatments include physical therapy to strengthen surrounding muscles, medications for pain and inflammation management, weight management to reduce joint pressure, and the use of orthotics or braces to support the knee. In some cases, corticosteroid or hyaluronic acid injections may provide temporary relief. These interventions aim to manage symptoms and improve function, delaying or avoiding the need for surgical intervention.
A joint replacement surgeon might assess several potential causes of hip avascular necrosis, including traumatic injury to the hip, chronic use of steroids, excessive alcohol consumption, and certain medical conditions like sickle cell anemia and lupus. Identifying the underlying cause is critical in determining the appropriate treatment approach, which may range from conservative management to joint replacement surgery in advanced cases.
Physical therapy is a cornerstone in managing low back pain associated with disc prolapse, focusing on strengthening the muscles surrounding the spine, improving flexibility, and promoting proper posture. A sports medicine specialist may implement customized exercise regimens to alleviate pain and support recovery. This non-operative approach aims to improve mobility, reduce pain, and prevent future disc issues, enhancing the patient's overall spinal health and function.
Trauma and fracture management techniques focus on restoring bone alignment and stability through methods like fixation with plates, screws, or rods. These techniques prioritize immediate injury repair. In contrast, joint replacement surgery involves replacing a damaged joint with a prosthetic to address chronic issues like arthritis or necrosis. While the former targets acute injuries, the latter is planned to alleviate long-term joint conditions and improve function over time.
Advancements in minimally invasive spinal procedures include the use of cutting-edge imaging technology for precise navigation, smaller incisions that minimize tissue damage, and the development of sophisticated instruments that allow for effective treatment of spinal conditions like disc prolapse. These innovations lead to shorter hospital stays, reduced postoperative pain, and faster recovery times, enabling patients to return to their daily activities with minimal disruption and improved overall outcomes.


.png)
.png)
.png)
.png)
.png)